Screenings, Protocols Successfully Reduce COVID-19 Risk for Urologic Cancer Patients
As patients delayed both routine and specialty health care in the first eight months of the COVID-19 pandemic, urologic surgeons at Penn State Cancer Institute observed an increase in advanced urologic cancer. To treat these cases while ensuring patient safety, urologic surgeons Dr. Jay Raman and Dr. Matthew Kaag with the Cancer Institute followed health screenings and testing protocols that have successfully reduced the risk of patients contracting COVID-19 while hospitalized.
“Our protocols allow us to identify those patients who have or are at risk for COVID-19 and to safely reschedule their surgery in a controlled manner so they can still receive the care they need without a prohibitive delay,” Raman says.
Mitigating COVID-19 risks
A retrospective analysis of 34 patients who received elective surgeries at four hospitals in Wuhan, China, during the incubation period of COVID-19 highlighted the potential danger of performing surgery on patients with active COVID-19 infections. Of the 34 patients studied, 100% developed pneumonia shortly after surgery, with abnormal findings on chest computed tomographic scans. Fifteen patients (44.1%) required Intensive Care Unit (ICU) admission during disease progression, and seven died after ICU admission. The mortality rate was 20.5%.¹
While these and other findings led the Commonwealth of Pennsylvania to suspend elective surgeries for a month last March, urologic cancer surgeries are essential. As a result, the Cancer Institute’s physicians and leaders focused on identifying patients with COVID-19 prior to surgical intervention.
“From the start, symptomatic patients were not eligible to have surgery,” Raman says. Starting on May 1, Penn State Health Milton S. Hershey Medical Center began requiring COVID-19 testing for all asymptomatic patients as well. Under the initial protocol, patients received a COVID-19 test three to five days prior to any procedure requiring anesthesia. Patients who lived outside the area and couldn’t access testing prior to admission received a same-day COVID-19 test upon admission. All patients testing positive for COVID-19 had their surgeries postponed for approximately 30 to 60 days after their initial date, provided a repeat COVID-19 test was negative.
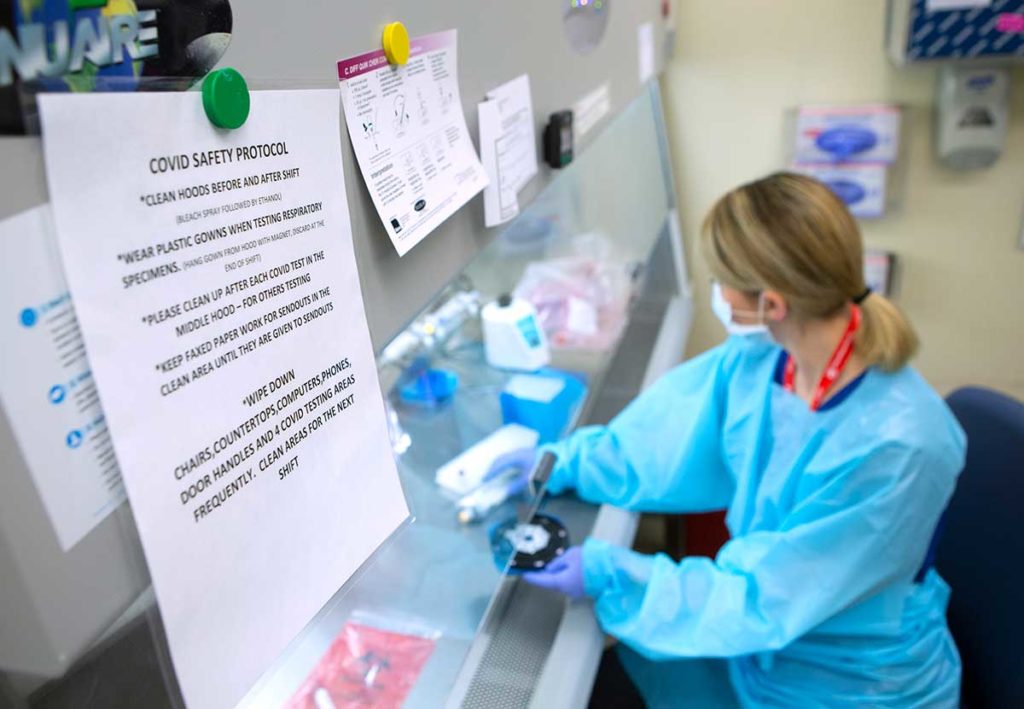
COVID-19 testing occurs for all Penn State Cancer Institute urologic surgery patients five days prior to a procedure date.
A retrospective review of 7,602 Hershey Medical Center surgery cases performed from May 1, 2020, to July 31, 2020, revealed that 54 patients tested positive for COVID-19 prior to surgery, a 0.7% positivity rate. Of the 792 urologic cancer surgeries performed at Hershey Medical Center during that same time frame, only three patients tested positive for COVID-19 prior to surgery, a 0.4% positivity rate.
“These results prove that we’re successful at safely navigating cancer patients requiring surgery while reducing the risk of COVID-19 sequelae,” Raman says.
Since August, a revised protocol set the mandatory preoperative COVID-19 testing time for five days prior to any procedure involving anesthesia to ensure appropriate testing turnaround times and workflow.
Observing increases in advanced urologic disease
As of June 30, 2020, because of concerns about COVID-19, an estimated 41% of U.S. adults had delayed or avoided medical care, including urgent or emergency care (12%) and routine care (32%)². Those national numbers had a local impact at Hershey Medical Center. “Patients we saw in subspecialty practices like urology informed us of challenges in getting routine and screening medical care due to barriers from COVID-19 and access to primary care offices,” Raman says.
To measure the impact of delayed care on urologic surgery patients, Raman and his urology colleagues compared Hershey Medical Center volume and diagnosis data from July 1, 2020, to Nov. 1, 2020, to data from the same dates the year prior. “We found that our surgical volume for both cancer and non-cancer urologic patients increased by about 19%, and we experienced a 24% increase in patients presenting with cancer conditions specifically,” Raman says.
Results of care delays observed by Hershey Medical Center’s urologic surgeons include increases in metastatic disease. “We’ve seen an uptick in patients needing more extensive
surgeries,” Kaag says. “I personally have performed more advanced kidney and testicular cancer procedures in the past three months than I normally see in three years.”
Timely patient referral can help catch and treat urologic cancers earlier. Penn State Cancer Institute takes multiple steps to keep patients safe from COVID-19, including performing initial assessments by phone, using the Penn State Health OnDemand app for telehealth visits when appropriate, conducting temperature screening for all patients seen in person and ensuring social distancing inside the clinic. “We do everything we can to make every interaction as safe as possible,” Kaag says.

Jay D. Raman, MD
Chair, Department of Urology
Professor, Department of Urology
Professor, Department of Surgery, Penn State Cancer Institute
Head, Robotic Surgery
Phone: 717-531-8887
Email: jraman@pennstatehealth.psu.edu
Fellowship: Urology, University of Texas Southwestern Medical Center, Dallas
Residency: General Surgery, New York-Presbyterian Weill Cornell Medical Center, New York; Urology, New York-Presbyterian Weill Cornell Medical Center, New York
Medical School: Weill Cornell Medicine/Cornell University, New York
Connect with Jay D. Raman, MD, on Doximity

Matthew G. Kaag, MD
Associate Professor, Department of Urology, Penn State Cancer Institute
Clinical Program Co-Leader in Genitourinary Oncology
Phone: 717-531-4475
Email: mkaag@pennstatehealth.psu.edu
Fellowship: Urologic Oncology/Surgery, Memorial Sloan Kettering Cancer Center, New York
Residency: Urology, Penn State Health Milton S. Hershey Medical Center, Hershey
Medical School: Penn State College of Medicine, Hershey
Internship: General surgery, Milton S. Hershey Medical Center, Hershey, Pa.
Connect with Matthew G. Kaag, MD, on Doximity
References
- Lei S., Jiang F., Su W., et al. Clinical characteristics and outcomes of patients undergoing surgeries during the incubation period of COVID-19 infection. EClinicalMedicine. 2020 Apr 5;21:100331 doi: 10.1016/j.eclinm.2020.100385
- Czeisler MÉ, Marynak K, Clarke KE, et al. Delay or Avoidance of Medical Care Because of COVID-19 Related Concerns – United States, June 2020. MMWR Morb Mortal Wkly Rep 2020;69:1250-1257. doi: http://dx.doi.org/10.15585/mmwr.mm6936a4
