New Celiac Clinic Offers Region’s Most Comprehensive Care
Penn State Health Milton S. Hershey Medical Center announces the opening of the Penn State Celiac Clinic, the first comprehensive celiac disease treatment program in central Pennsylvania. Led by Kofi Clarke, MD, director of the clinic and chief of the Division of Gastroenterology at the Milton S. Hershey Medical Center, the program offers comprehensive care across the celiac spectrum, from celiac disease and gluten intolerance to seronegative celiac disease and patients with self-imposed gluten-free diets.
“It is amazing to see how rapidly the program has grown in such a short amount of time,” says Dr. Clarke, who previously ran a similar program in Pittsburgh. “We have been collecting data since we opened in 2017 and will begin formal research into quality-of-life outcomes for celiac patients later this year. We also look forward to beginning community outreach and awareness events this summer.”
The clinic offers full-circle clinical diagnostics and care for patients who wish to be followed at Hershey Medical Center, including confirmatory or exploratory diagnostic testing, nutrition counseling, genetic testing and sessions on gluten-free lifestyles for individuals who have no medical reason to avoid gluten. They also offer evaluation of symptoms that may be caused by gluten intolerance, seronegative celiac disease or other common causes of gastrointestinal distress that may mimic the symptoms of celiac.
In addition to celiac experts Dr. Clarke and Emmanuelle Williams, MD, who are specialist gastroenterologists at the Penn State College of Medicine, patients can see a clinic psychiatrist and a registered dietitian with a specialty in celiac and gluten-free diets. The clinic’s nutritionist services are open to all patients, whether or not they see Drs. Clarke or Williams for their celiac care.
“We have many patients who come in for the nutrition education alone or just for a comprehensive diagnostic work-up,” Dr. Clarke explains. “Once we provide the needed assessment, we work with them to create a treatment plan that can be directed by their local gastroenterologist. With that, they are able to follow up with us only as needed for clarification or additional assistance.”
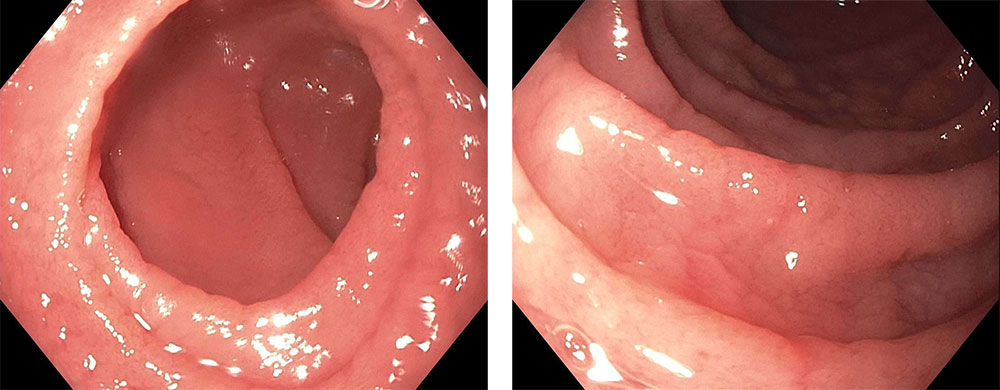
FIGURE 1. Close-up endoscopic findings in a Penn State Celiac Clinic patient with celiac disease
After clarification or confirmation of the diagnosis, adoption and maintenance of a true gluten-free diet is more complicated than just avoiding gluten, Dr. Clarke says. He firmly believes the disease’s nutrition-focused management requires frequent education and collaboration with a specialized dietitian.
“Many patients are just told to start a gluten-free diet, and that’s too simplified,” Dr. Clarke says. “Our nutritionist works through the details with patients, educates them and make adjustments to their care plans, assesses them for nutrient deficiencies and bone disease, teaches them how to read nutrition labels at the grocery store and talks with them about eating with their non-gluten-free spouses and out at restaurants.”
Comprehensive clinics such as the Penn State Celiac Clinic are increasingly important because of the rise in incidence of gluten intolerance as well as misleading statements about gluten-free diets popularized in the media, Dr. Clarke says.
“There are a lot of misconceptions about gluten and a lot of components in gluten-containing foods that could be the problem, rather than a true celiac diagnosis or gluten intolerance,” Dr. Clarke says. “We have people come to the clinic who have been gluten-free for years assuming they are intolerant, and they suddenly decide to find out if they actually are. The majority of those patients have been able to return to a normal diet because it wasn’t celiac disease or a gluten intolerance at all.”
Dr. Clarke suggests the Celiac Clinic as a particularly valuable resource for:
- Patients with a confirmed diagnosis of celiac disease or suspected gluten intolerance, but lack of response to a gluten-free diet
- Patients for whom the diagnosis is in doubt or who wish to receive comprehensive diagnostic blood tests
- Patients who may be experiencing clinical problems in addition to their celiac disease
- Patients looking for additional guidance on following a gluten-free diet
- Patients who need assistance coping with the social and emotional aspects of their diagnosis and diet
“Our program is totally accessible—patients don’t need special referrals to come see us, and they are under no obligation to keep coming here for follow-ups if they’re already managed by a gastroenterologist closer to home,” Dr. Clarke says. “We provide the needed assessment and education, usually in a single visit, and provide them with a detailed plan to take home. Our goal is to have patients be successful at managing their disease.”

Kofi Clarke, MD, FACP, FRCP, AGAF
Division Chief, Gastroenterology and Hepatology, Penn State Health Milton S. Hershey Medical Center
Phone: 717-531-4950
Email: kclarke@pennstatehealth.psu.edu
Fellowship: Gastroenterology and hepatology, University of Pittsburgh Medical Center, Pittsburgh, Pa.; Research Fellowship: Michigan State University, East Lansing, Mich.
Residency: Internal medicine, Temple University School of Medicine, Western Pennsylvania Hospital, Pittsburgh, Pa.; Gastroenterology and hepatology, Royal College of Physicians, London
Medical School: University of Ghana Medical School, Ghana
Postgraduate: Medicine, Gastroenterology and hepatology, Imperial College, London
Connect with Kofi Clarke, MD, FACP, FRCP, AGAF, on Doximity

