New Subspecialty of Adult Congenital Heart Disease Now Available to Address Unique Cardiac Needs
Due to advances in treatment and technology, more patients than ever before who are born with congenital heart disease (CHD) are living into adulthood. For the first time, there are more adult than pediatric CHD patients, with the number of adult cases in the U.S. estimated at 1.3 million.1 The management of these patients is so complex that a new subspecialty of adult congenital heart disease (ACHD) is now available for certification by the American Board of Medical Specialties. Penn State Heart and Vascular Institute has long recognized the complex needs of this growing population, and started a program for adult congenital heart disease (PACHD) in 1991, which is directed by William Davidson, Jr., MD.
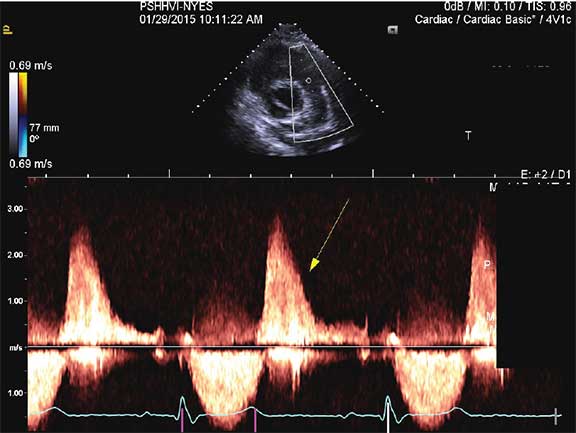
Color Doppler image of severe pulmonic insufficiency, commonly found in Tetralogy of Fallot patients.
Currently, the PACHD has three ACHD providers, all of whom are board certified, having sat for the first-ever ACHD subspecialty boards in October 2015. These specialized clinicians provide 24/7 coverage to all ACHD inpatients, and provide personalized, consistent care to complex patients, most of whom have six to 10 active medical conditions. Problems associated with congenital heart disease include valve disease, heart failure, arrhythmias, aortic and other vascular diseases; pulmonary, renal and liver disease; and a history of multiple surgeries. For example, one of the fastest growing ACHD patient populations have tetralogy of Fallot (ToF).2 This condition requires complex intracardiac “corrective” surgery. A common late consequence is pulmonary valve insufficiency (PI), which can lead to right ventricular dysfunction and sudden death.2 PI is a common lesion in this population that is often missed with conventional testing, according to Dr. Davidson. All ACHD patients require lifelong follow-up and regular visits to an ACHD specialist.
As the patients age, so does the natural history of CHD; many adult patients have problems not detected in childhood or adolescence. The PACHD also focuses on the growing burden of arrhythmia and its concomitant risk of sudden death, the role of the right ventricle in heart failure among this population and the importance of interventional cardiology, as opposed to open surgery, whenever possible.
Guidelines established at the 32nd Bethesda Conference of the American College of Cardiology (ACC), which Dr. Davidson co-authored, state that “all adults born with complex congenital heart defects should be seen at specialized ACHD care centers.”3 Unfortunately, only about 10 percent of adult CHD patients seek appropriate care from adult congenital cardiologists, and estimates put the number of adults with CHD who receive any sort of cardiovascular care at just below half.4 Dr. Davidson also points out that Canadian data have shown having treatment dedicated to adult congenital heart disease reduced hospitalizations by 4 percent per year and can improve outcomes overall in this population.5 “Specialty cardiovascular care is so key,” he says, “and helps us determine if patients can return to the care of their primary cardiologists or need specialized care throughout their lives to prevent unnecessary complications and premature death.”

William R. Davidson Jr., MD
Professor, Medicine
Director, Program for Adults with Congenital Heart Disease
Phone: 717-531-7473
Email: wdavidson@pennstatehealth.psu.edu
Fellowship: Cardiology, University of Rochester Medical Center, Rochester, N.Y.
Residency: Internal medicine, Pennsylvania Hospital, Philadelphia, Pa.
Medical School: University of Pennsylvania School of Medicine, Philadelphia, Pa.
Connect with Division of Cardiology on Doximity
References:
- Moodie D. Adult Congenital Heart Disease: Past, Present, and Future. Tex Heart Inst J. 2011; 38(6): 705–706.
- Suleiman T, Kavinsky CJ, Skerritt C, Kenny D, Ilbawi MN, and Caputo M. Recent Development in Pulmonary Valve Replacement after Tetralogy of Fallot Repair: The Emergence of Hybrid Approaches. Front Surg. 2015;2:22.
- http://www.achaheart.org/resources/ for-patients/achd-care-guidelines.aspx. Accessed September 24, 2015.
- Nainggolan L. Adult Congenital Heart Disease a New Subspecialty. Heartwire from Medscape.com. December 12, 2012.
- Islam S, Yasui Y, Kaul P, Marelli AJ, Mackie AS. Congenital Heart Disease Hospitalizations in Canada: A 10-Year Experience. Can J Cardiol. 2015 Jun 4. pii: S0828-282X(15)00404-3.
