Penn State Health Takes Multidisciplinary Approach to Treating Skull Base and Pituitary Tumors
Skull base tumors and tumors affecting the pituitary gland can cause a wide range of serious symptoms and can be life-threatening. Both cancerous and benign tumors need diligent evaluation and treatment by an experienced team to determine the best treatment plan for each individual patient.
High-Stakes Surgery
Skull base surgery, sometimes referred to as cranial base surgery, takes place at the bottom of the skull near the base of the intracranial cavity. The anterior skull base separates the nose and sinuses from the brain and spinal fluid, while the lateral skull base separates the ear, hearing and balance organs from the brain and spinal fluid.
All along the skull base lie critical structures, including blood vessels and cranial nerves that are essential to vision, facial movement, hearing, balance, swallowing and speech, among other functions. Skull base surgery is a highly specialized set of techniques to remove or repair lesions along this bony junction.
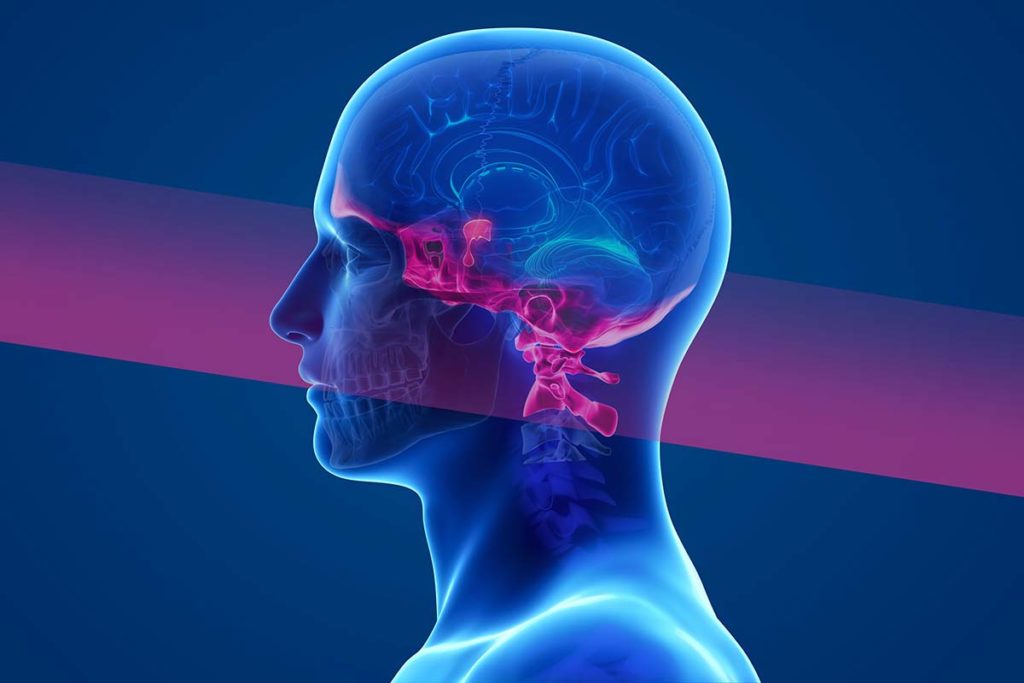
The skull base, or bottom part of the skull, which is highlighted, is a complex anatomic region where multiple critical neurovascular structures pass by or through. Above the skull base sits the pituitary gland, also highlighted. The pituitary gland is the master regulator of the body’s production of several hormones critical for normal function.
The pituitary gland is located in the skull below the brain and above the nasal passages. Known as the “master gland,” it releases hormones regulating various functions in the body and stimulates other glands to secrete hormones.
Most pituitary tumors are adenomas. Despite being benign, they can result in significant health problems by causing the pituitary gland to produce too much or too little of certain hormones or by pressing on the optic nerve. A pituitary tumor can cause a wide range of symptoms, including vision problems, headaches, infertility, erectile dysfunction and mood changes.
“It’s always humbling to consider the high stakes,” said Dr. Neerav Goyal, associate professor of Otolaryngology ― Head and Neck Surgery and director of head and neck surgery at Penn State Cancer Institute. “The skull base region contains a complex anatomy of vessels and nerves where injury of these structures can lead to stroke or the loss of vision. Fortunately, having an experienced and collaborative team of surgeons that is cognizant of the risks helps keep these concerns to a minimum. ”
For each patient with a skull base tumor or pituitary tumor, the multidisciplinary care team at Penn State Health Milton S. Hershey Medical Center creates a plan to effectively treat the tumor and preserve function and quality of life. The team treats a range of conditions ranging from the relatively common (pituitary adenoma, meningioma and schwannoma, for example) to the rare (craniopharyngioma and esthesioneuroblastoma, for instance).
Depending on a patient’s initial symptoms, they’re typically first referred to a neurosurgeon, otolaryngologist, oculofacial plastic surgeon or ophthalmologist, who determines what tests are needed. Those tests can include computed tomography and magnetic resonance imaging of the head and face.
Once a diagnosis is made, the patient sees other members of the team, depending on the location and pathology of the lesion. This may include neurosurgeons, head and neck surgeons, radiation and medical oncologists, oculofacial plastic surgeons, ophthalmologists and otologists. All of these physicians meet and discuss each patient to create a treatment plan that is both effective and prioritizes preservation of hormones, nerves and blood vessels whenever possible.
“Penn State Health is really the only center in the region that brings together fellowship-trained experts in these subspecialty areas with the framework, facilities and technology to tackle these pathologies at the highest level,” said Dr. Brad Zacharia, assistant professor of neurosurgery, co-director of the neuro-oncology program and director of brain tumor and skull base surgery at Penn State Health.
The team holds regular tumor board meetings to discuss complex cases. These meetings bring together the surgical team as well as radiologists, pathologists and oncologists to craft a comprehensive treatment plan. Based on the tumor location, type and other factors, a patient’s plan may include minimally invasive endoscopic surgery, radiosurgery, open surgery, radiation, chemotherapy, reconstructive surgery or a combination of these techniques.
“Skull base and pituitary tumor care is done jointly with neurosurgery and otolaryngology, as well as others. It’s a very collaborative process,” said Dr. Meghan Wilson, assistant professor in the Department of Otolaryngology ― Head and Neck Surgery.
Dr. Wilson is one of the few U.S. experts trained in both adult and pediatric skull base surgery. “The vast majority of the country’s skull base surgeons treat adults,” she said. “When a child comes along, they are often not used to operating on or caring for a person of that size. That’s one of the unique things about our program ― we’re experienced in treating pediatric patients as well as adults.”
Leading-Edge Techniques
Two or three decades ago, approaching tumors in these areas required a craniotomy. “This meant taking off half the skull, retracting the brain and taking out the tumor,” Dr. Goyal said.
As different technologies have hit the market, surgeons have been able to access many of these tumors through less invasive approaches. Today, the team at Penn State Health uses a variety of approaches to remove tumors through the nose, the space adjacent to the eye, the ear or just behind the ear using small incisions.
The most common surgery for pituitary tumor is the transsphenoidal approach, which is done through the sphenoid sinus, a hollow space in the skull behind the nasal passages and below the brain. At Penn State Health, it’s most commonly done with an endoscope inserted through the nose. With this noninvasive technique, no part of the brain is touched, and there is no visible scar.
The skull base and pituitary tumor care team also offers the most advanced surgical radiation technology available for the brain, the Leksell Gamma Knife Icon. This noninvasive, ultraprecise approach concentrates up to 192 radiation beams on the tumor, sparing healthy brain tissue. During surgery, the team uses image-guided technology to assess the tumor and its location relative to important structures such as nerves and blood vessels.
“When we’re dealing with these critical structures at the base of the skull, accuracy becomes paramount,” Dr. Zacharia said. “The Gamma Knife has really changed the way we’ve managed patients. Prior to radiation techniques like this, the surgeries were much more radical because there were no other options. Now we’re able to sculpt the radiation in exquisite detail to converge on our target and deliver a high dose. Oftentimes, a single treatment to these pathologies is enough.”
Penn State Health is a university health system. As such, its skull base and pituitary tumor care team conducts research to advance the field, sometimes in surprising ways. Dr. Goyal recently published a study in JAMA Otolaryngology–Head & Neck Surgery about the mental health effects of a head and neck cancer diagnosis. “We’re all actively doing research to try to keep on pushing the needle forward,” he said.
Reference:
Brassfield, Mike. Illuminating a Path to Enhanced Bladder Cancer Detection. MD News Central Pennsylvania Edition. Dec. 2019. centralpennsylvania.mdnews.com/milton-s-hershey-medical-center-skull-base-surgery-team-comprehensive-care-close-home Accessed Dec. 4, 2019.

Neerav Goyal, MD, MPH, FACS
Chief, Division of Head and Neck Oncology and Surgery
Associate professor and vice chair for quality and safety, Department of Otolaryngology ─ Head and Neck Surgery
Associate professor, neurosurgery and public health sciences, Penn State College of Medicine
Phone: 717-531-6822
Email: ngoyal1@pennstatehealth.psu.edu
Fellowship: Surgical oncology, head and neck, Massachusetts Eye and Ear Infirmary, Harvard Medical School, Boston
Residency: Otolaryngology, and Otolaryngology – Head and Neck Surgery, Penn State Health Milton S. Hershey Medical Center
Medical School: Jefferson Medical College of Thomas Jefferson University, Philadelphia
Connect with Neerav Goyal, MD, MPH, FACS, on Doximity

Meghan Wilson, MD
Assistant Professor of Surgery, Department of Otolaryngology – Head and Neck Surgery
Phone: 717-531-6822
Email: mwilson18@pennstatehealth.psu.edu
Fellowship: Cranial base surgery, Northwell Health, New York; Pediatric otolaryngology, Children's Hospital of Philadelphia
Residency: Otolaryngology, Louisiana State University Medical Center, New Orleans; Otolaryngology – Head and Neck Surgery, Louisiana State University Medical Center, New Orleans
Medical School: Louisiana State University School of Medicine, New Orleans
Connect with Meghan Wilson, MD, on Doximity

Brad E. Zacharia, MD, MS
Associate Professor of Neurosurgery and Otolaryngology
Co-director, Neuro-Oncology Program
Director, Brain Tumor and Skull Base Surgery, Penn State Health Milton S. Hershey Medical Center
Phone: 717-531-4177
Email: bzacharia@pennstatehealth.psu.edu
Fellowship: Neurosurgical Oncology, Memorial Sloan Kettering Cancer Center, New York
Residency: Neurological Surgery, New York Presbyterian Hospital – Columbia University, New York
Medical School: Columbia University College of Physicians and Surgeons, New York
Connect with Brad E. Zacharia, MD, MS, on Doximity

